What is a general Biomechanical Assessment?
You don't need to be an athlete to benefit from a biomechanical assessment, as many issues arise from your normal activities. You use your feet alot in any given day and over time this can lead to issues that seem to appear from nowhere.
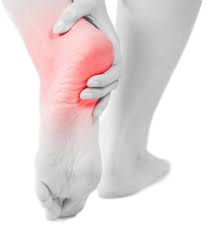
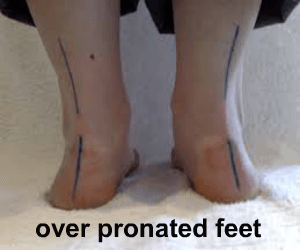
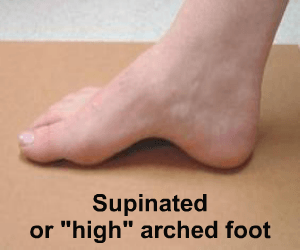
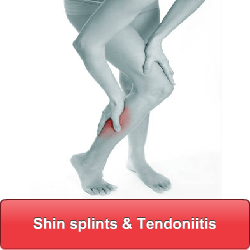
The truth is these problems can appear through normal wear and tear. Small anomalies in your foot, leg and body alignment can lead to minor stresses and micro trauma which over the years result in what appears like a spontaneous injury. We run through some examples of these below
A biomechanical assessment is a specialist assessment we undertake in our clinics in Hamilton, Glasgow and Aberdeen. It involves a full medical history, assessment of joint ranges and muscle powers and video gait analysis. Find out more in depth detail below about our biomechanical assessment service and the conditions that can benefit from a biomechanical assessment.
What are the benefits?
The reality of foot, leg or knee pain is that it rarely happesn by accident. More often than not, small biomechanical anomalies are present which go unnoticed for many years and then eventually present as "wear and tear" type injuries or when we try to increase our activity placing the body under greater biomechanical forces and stress.
Our biomechanical assessment clinics are delivered by genuine experts in their field and work alongside Orthopaedic surgeons, Physiotherapists, Podiatrists and Orthotists all working together to take a holistic approach to your particular issues.

Four stages of assessment
The general biomechanical assessment consists of 4 main stages: Defining the problem (clinical history) , Static alignment and range of motion assessment, Dynamic alignment and video gait analysis, and finally, Patient feedback, diagnosis and treatment prescription.
Defining the Problem
The most important part of the biomechanical assessment is listening to the patient to understand the problem. It is vital that we understand the issue you have come to see us about from your persective.
Often other clincians are keen to give patients their view of the problem when really they are not the person living with it. Instead we need to hear it from your side to understand how your problem impacts on you.
We take a history of the current and previous issues you may have as well as a full medical history to inform what may be important factors to consider before starting our assessment. Equally, we need to understand what the patient is expecting from us.
Static Alignment & Range of Motion
Once we have have taken a history we assess your body alignment including, your feet/ankles. legs, knees, hips, spine and shoulders usually standing to check for any alignment issues. We then also assess the alignment and movement of your joints when moved (passive and active movement) to check against normal limits.
Any signs of potential alignment issues, muscle weakness or imbalances are recorded and discussed with you as the assessment takes place.
Sometimes it easier if you bring shorts or leggings, however it is not always necessary dependant on where your issues are
Dynamic Alignment & Video Gait Analysis
Sometimes the problem you have with the way you walk (your gait) is not always obvious to the human eye. This is why after the assessment of your alignment we look to see what happens when you move.
This in essence a way of confirming our findings from the static aligment and range of movement assesment. your gait is analysed using video gait analysis equipment to allow us to look in more detail at exactly what happens when you walk or run.
Often with biomechanical issues you will see compensatory movements or "trick" movements that your body adopts (without you being aware of it) to try to overcome your underlying problem. Video gait analysis as part of the assessment helps identify these.
Patient Feedback, Diagnosis & Prescription
The final part of the process is feeding back the findings of the biomechanical assessment through slow motion video gait analysis and the assessment findings.
A full and honest view of the possible treatment we can offer you, or alternatively we will advise on the possibility of us referring you to other members of our team for treatment.
For any orthotics/insoles that we may prescribe we make these on site and discuss your options as to how these may may be made to best fit your needs.